About the Author
Things to do on Long Island
Tomorrow, 9 am
Tomorrow, 11 am
July 19, 10 am
July 26, 7 pm
BoLI Spotlight
 The Shed: Inside the 2025 Best Outdoor Dining restaurant
The Shed: Inside the 2025 Best Outdoor Dining restaurant Planet Play: Inside the 2025 Best Arcade on Long Island
Planet Play: Inside the 2025 Best Arcade on Long Island Teresa’s Lunch Box: Inside the 2025 Best Deli on Long Island
Teresa’s Lunch Box: Inside the 2025 Best Deli on Long Island Long Island Children’s Museum: Inside the 2025 Best Theatre Arts Center
Long Island Children’s Museum: Inside the 2025 Best Theatre Arts Center Looney Tunes: Inside the 2025 Best Record Store on Long Island
Looney Tunes: Inside the 2025 Best Record Store on Long Island
Latest News
 Long Island housing nonprofit fights $1m Trump cuts
Long Island housing nonprofit fights $1m Trump cuts New Hyde Park Chamber, Lions Club honor Gladiator Fund at annual golf outing
New Hyde Park Chamber, Lions Club honor Gladiator Fund at annual golf outing Audit finds Health Dept. slow to inspect violations at Long Island elder care facilities
Audit finds Health Dept. slow to inspect violations at Long Island elder care facilities LI water providers awarded $250M to remove PFAS contaminant from drinking supply
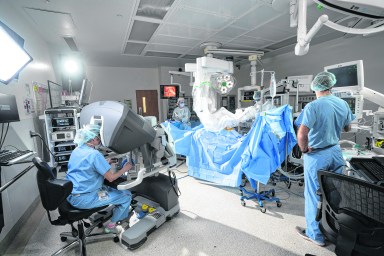
LI water providers awarded $250M to remove PFAS contaminant from drinking supply Northwell sees 1st AI-assisted hip replacement surgery in the country
Northwell sees 1st AI-assisted hip replacement surgery in the country